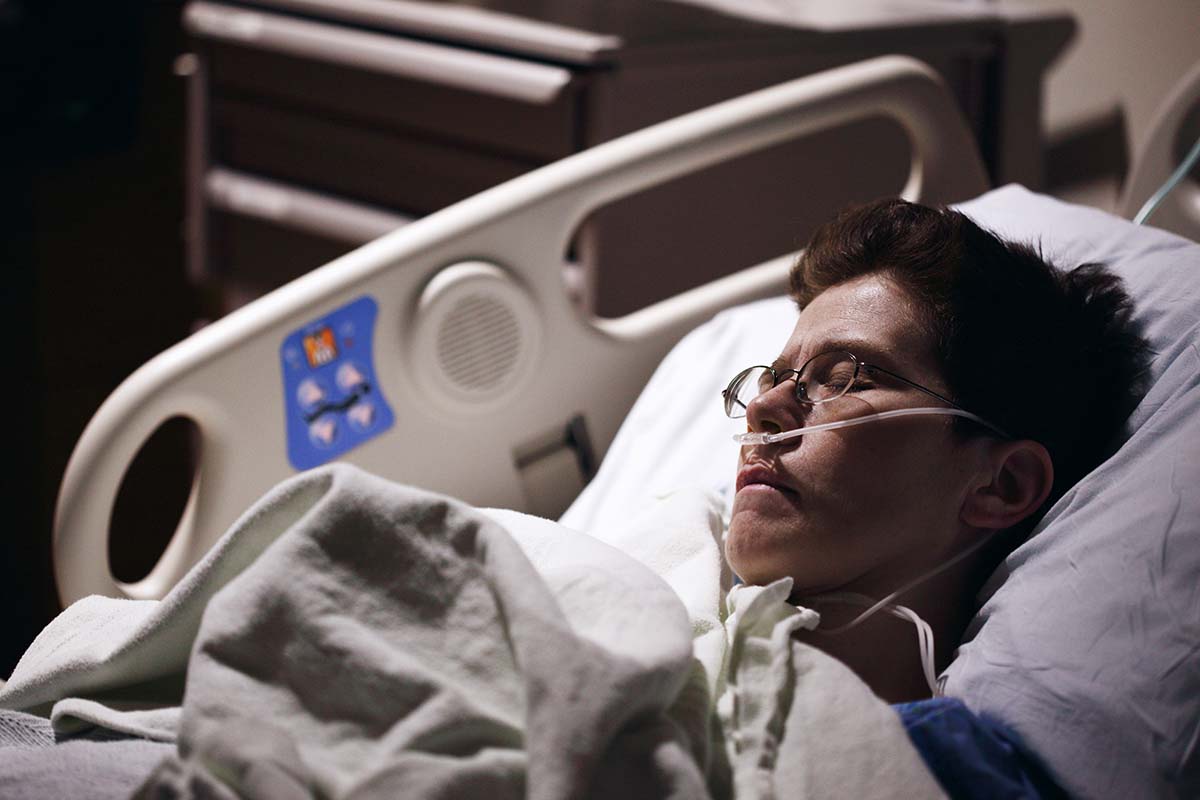
Regarding healthcare, accurate and timely diagnosis is crucial for effective treatment and improved patient outcomes. However, medical misdiagnosis is an unfortunate reality that can profoundly affect patients’ lives.
Whether it’s a delayed diagnosis, an incorrect assessment, or a failure to recognize symptoms, medical misdiagnosis can significantly impact a patient’s quality of life. By understanding the challenges patients face due to misdiagnosis, we can work towards bettering medical practices and ensuring patients receive the care they truly need.
How Medical Misdiagnosis Affects Patients’ Quality of Life: Legal and Ethical Implications
Patients who have suffered harm due to misdiagnosis may pursue medical malpractice claims, seeking compensation for their physical and emotional damages. These legal battles can be lengthy, expensive, and emotionally draining for all parties involved, especially regarding cancer.
Having legal support for cancer misdiagnosis should be mandatory for anyone going through such a case. From an ethical standpoint, misdiagnosis raises questions about the responsibility of healthcare providers to deliver accurate diagnoses and the measures that should be taken to prevent such errors. Addressing these ethical concerns is crucial to improving patient safety and ensuring accountability within the healthcare system.
The Emotional Toll of Misdiagnosis
Receiving an incorrect diagnosis can be a deeply traumatic experience for patients and their families. Emotionally, patients may go through a rollercoaster of feelings, ranging from confusion and frustration to anxiety and fear.
The uncertainty surrounding their health condition and treatment plan can increase stress and mental anguish, negatively impacting their overall well-being. Coping with the emotional aftermath of a misdiagnosis can be daunting, often requiring the support of mental health professionals and a strong social network.
Physical Consequences and Delayed Treatment
A misdiagnosis can delay receiving the appropriate treatment for the actual medical condition. These delays can result in the progression of the disease or illness, causing further harm to the patient’s health.
For instance, a patient misdiagnosed with a less severe condition might not receive the necessary interventions for a more serious ailment, leading to irreversible damage or even life-threatening situations. Additionally, unnecessary treatments and medications prescribed for the misdiagnosed condition can introduce new health risks, exacerbating the patient’s health issues.
Financial Strain and Healthcare Costs
The financial burden of medical misdiagnosis can be overwhelming for patients and their families. The cost of repeated medical visits, diagnostic tests, and treatments can quickly add up, especially if the misdiagnosis persists for an extended period.
Moreover, misdiagnosis-induced complications may necessitate additional medical interventions and prolonged hospital stays, further straining the family’s finances. In some cases, patients may even face loss of income due to extended leave from work, making it even more challenging to cope with the financial implications of misdiagnosis.
Loss of Trust in the Healthcare System
A significant consequence of medical misdiagnosis is the erosion of trust in the healthcare system. When patients experience misdiagnosis, they may question the competence of their healthcare providers and the reliability of medical institutions.
This loss of trust can lead to hesitancy in seeking medical care, avoidance of recommended screenings, and delays in reporting symptoms, potentially worsening their health outcomes. Restoring faith in the healthcare system requires transparency, improved communication between healthcare providers and patients, and a commitment to learning from past misdiagnoses.
Long-Term Psychological Effects
The repercussions of medical misdiagnosis often extend far beyond the initial experience. Patients who have endured the trauma of being misdiagnosed may develop long-term psychological effects.
These may include a profound sense of mistrust in the medical system, persistent anxiety about their health, and post-traumatic stress disorder (PTSD). Even after receiving a correct diagnosis and appropriate treatment, patients may struggle with intrusive thoughts and fears related to their past misdiagnosis. Such psychological distress can impede their ability to engage in daily activities, maintain relationships, and overall diminish their quality of life.
Impact on Relationships and Social Life
Medical misdiagnosis can disrupt a patient’s personal and social life, leading to strained relationships and isolation. Family members and friends may struggle to understand the complexities of the misdiagnosis, which can create tension and communication breakdowns.
Additionally, patients who experience ongoing health challenges due to misdiagnosis might be unable to participate in social gatherings and events, further isolating them from their support networks. The loss of social connections and the inability to engage in previously enjoyed activities can contribute to feelings of loneliness and depression, compounding the negative effects on their overall well-being.
Medical misdiagnosis is a multifaceted issue with profound consequences for patients, impacting their physical health, emotional well-being, financial stability, and social relationships. The emotional toll of receiving an incorrect diagnosis and delayed treatment can lead to severe health complications and increased healthcare costs.
Moreover, the loss of trust in the healthcare system can exacerbate patients’ reluctance to seek timely medical care, further compromising their health outcomes. To mitigate the impact of medical misdiagnosis, healthcare providers and institutions must prioritize diagnostic accuracy through ongoing education, advanced technologies, and improved communication with patients.