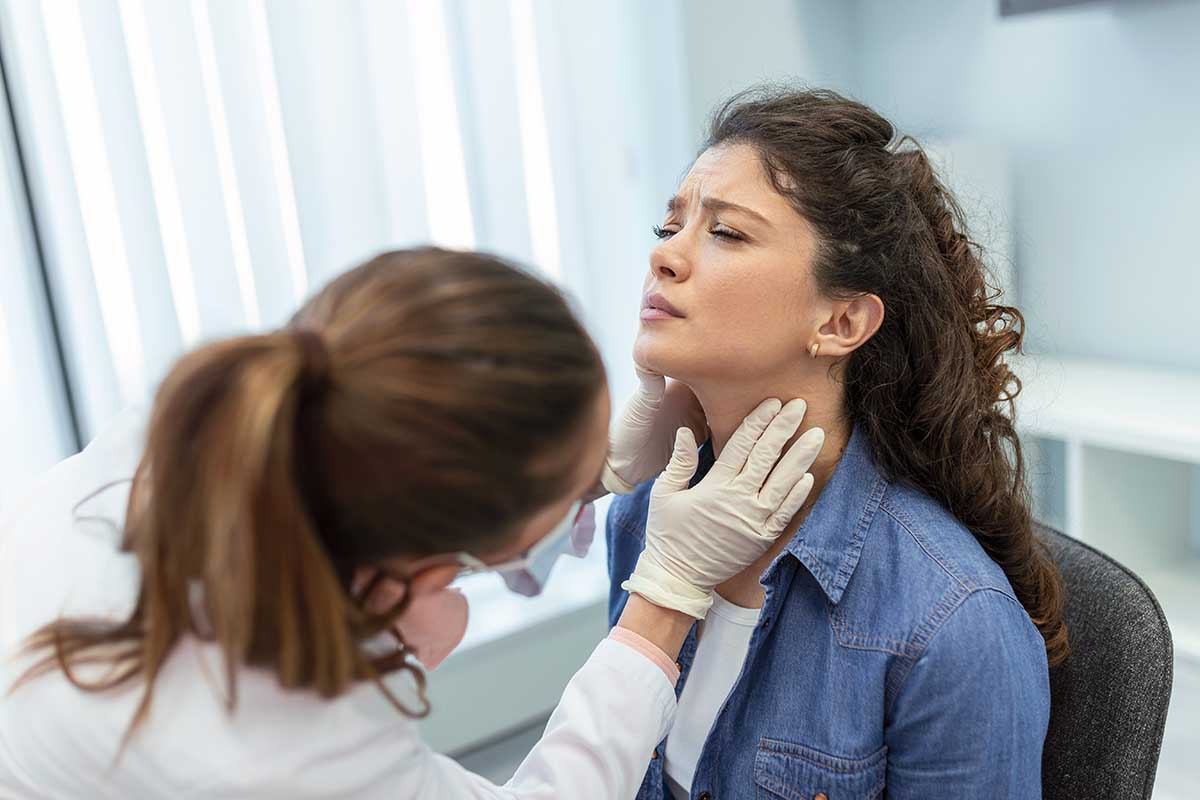
PTSD and Self-Medication: Understanding the Relationship
Post-Traumatic Stress Disorder (PTSD) is a mental health condition that can develop after exposure to a traumatic event. With PTSD, you can often grapple with intrusive memories, heightened anxiety, and a persistent sense of threat. This can quickly have a detrimental impact on your daily life.
One coping mechanism that frequently emerges as a result of PTSD is self-medication. This comes as a result of attempting to alleviate symptoms through substance use. There are various treatment options for drug addiction. In addition, it also helps to understand the relationship between PTSD and self-medication.
Understanding PTSD
A good starting point would be to understand what often triggers PTSD. It arises from exposure to traumatic incidents such as combat, sexual assault, natural disasters, or accidents. The condition manifests through symptoms like flashbacks, nightmares, hypervigilance, and emotional numbness. The emotional toll of these experiences can be overwhelming. This can then lead to the prospect of seeking relief and escape from these distressing thoughts and emotions.
Self-medication as a coping mechanism
If you are suffering from PTSD, you may turn to substances like alcohol, drugs, or prescription medications to manage your symptoms. Self-medication can temporarily provide a sense of relief, helping to numb emotional pain and create a semblance of normalcy. Unfortunately, this coping strategy often leads to a cycle of dependence, exacerbating the original issues while introducing new challenges at the same time.
Underlying factors
Several factors contribute to the link between PTSD and self-medication. The attempt to regain control over your emotions, the opportunity to ease anxiety, and the idea that you can escape from traumatic memories can drive you to substance use.
The fundamental problem is that the co-occurrence of PTSD with conditions like depression and anxiety further intensifies the desire for relief. This creates a vulnerable environment for self-medication.
The biological impact
The neurological impact of trauma plays a significant role in the connection between PTSD and self-medication. Traumatic experiences can alter brain chemistry, affecting neurotransmitters related to mood regulation.
This imbalance may drive you to seek substances that temporarily restore a sense of equilibrium. Unfortunately, this relief is short-lived and can lead to a dangerous cycle of dependence.
Breaking the cycle
Recognizing the intertwined nature of PTSD and self-medication is crucial for effective treatment. Instead of merely addressing the symptoms, a comprehensive approach involves addressing the root causes of trauma.
Therapy options such as cognitive-behavioral therapy (CBT) and eye movement desensitization and reprocessing (EMDR), aim to rewire maladaptive thought patterns and process traumatic memories.
These treatments could prove to be the catalyst for breaking the cycle.
Integrated treatment
Effective treatment involves an integrated approach that combines therapy, medication, and support networks. Medications may be prescribed to alleviate specific symptoms, while therapy provides a platform for helping to explore the underlying trauma and develop healthier coping mechanisms. It is also wise to establish a strong support system, whether through friends, family, or support groups. This is vital in promoting lasting recovery.
The relationship between PTSD and self-medication is complex and multifaceted. Recognizing the interconnected nature of these issues is the first step toward breaking the cycle. You will need a supportive environment and professional guidance to navigate the challenging journey of healing from PTSD and breaking free from that cycle of self-medication.