Risk of Pulmonary Embolism: What You Need to Know
The risk of pulmonary embolism is a blockage located in the pulmonary artery in your lungs. Most of the time, the blockage is a blood clot that has traveled from the legs. Clots could come from somewhere else in the body, but that is rare.
Who is at Risk
As with most disorders, you are at a higher risk for PE if you or members in your family have had PE or venous blood clots in the past. Other factors may increase the likelihood that you will experience a pulmonary embolism. Heart diseases, like heart failure and heart attacks, increase the risk of clotting. Certain cancers can also cause clotting, especially if you have gone through chemotherapy. Pancreatic, ovarian, and lung cancer may cause an embolism along with the treatment for these cancers.
Unsurprisingly surgery can also be the cause of PE. It is common for clots to form during surgery, which is why usually before and after surgery, you are given blood thinners to stop clotting. Other factors include being confined to a bed for an extended period, smoking, being overweight, being confined to a small space, and pregnancy.
Signs of a Pulmonary Embolism
If you are at risk, you should know what to look for when dealing with PE. Some of the symptoms of PE are shortness of breath, chest pain that is reminiscent of a heart attack, a cough with bloody sputum. The chest pain will usually flare up when you exert yourself, and it won’t go away after you get some rest.
Other signs you should be aware of include leg pain or swelling in the calf, clammy skin, fever, and rapid or irregular heartbeat.
How to Lower Your Risk
There are five things you can do that might lower your chances of developing blood clots.
- Blood thinners or anticoagulants keep your blood from forming clots. A doctor usually prescribes this type of medication before or after surgery to prevent clotting. You may also have to take it when you return home. If you have been hospitalized because of a stroke or heart attack, blood thinners will be prescribed to you to stop a PE from forming.
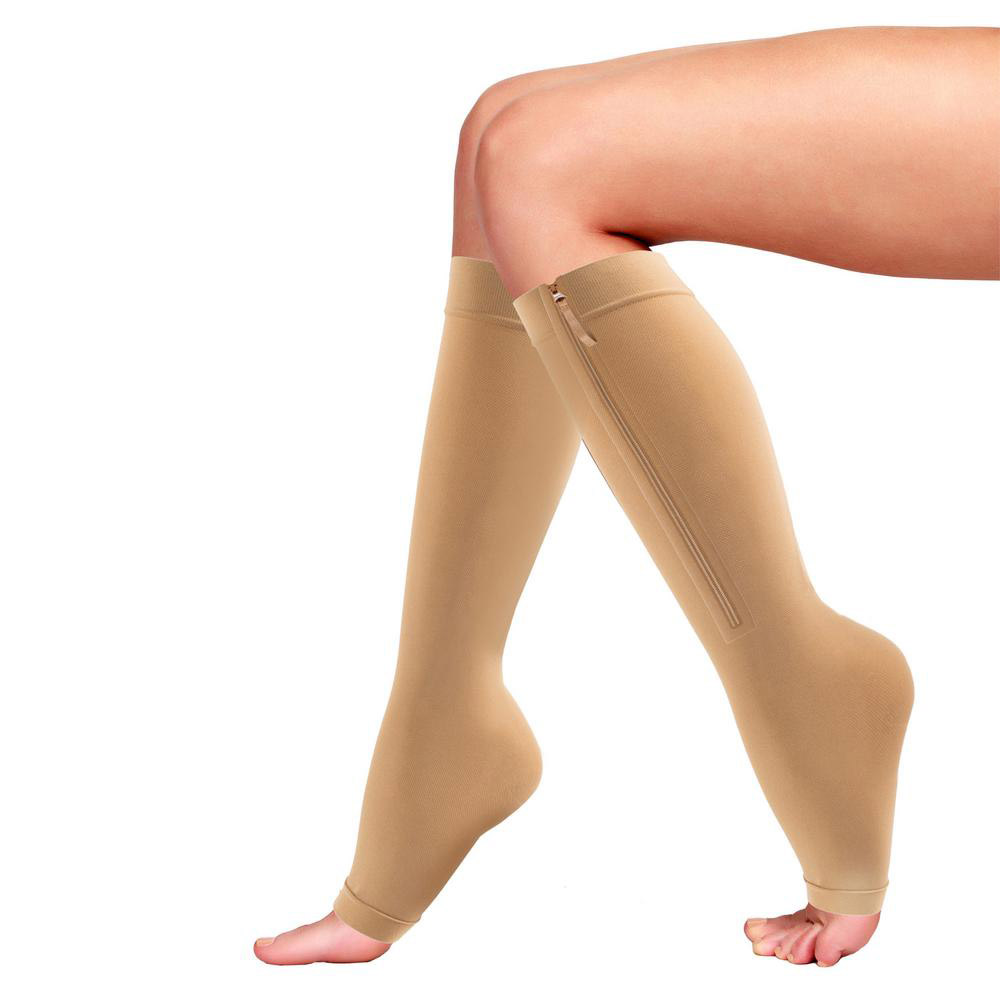
- Compression socks or stockings can be worn to help prevent PE. You should wear compression socks or pneumatic compression. Compression socks are long socks that squeeze and put extra pressure on your legs. They will help to keep the blood flowing easily through the veins in your legs. With pneumatic compression, you wear thigh-high or calf-high cuffs that inflate and deflate every few minutes to massage and squeeze the veins in your legs that will improve blood flow.
- Exercise can also help prevent PE. If you sit for long periods of time or have been bedridden, blood could pool in your legs and cause a clot. The movement will help to stop this from happening. Walk around as often as possible to keep your blood flowing.
- Stretching is another activity you can do to prevent PE. If you have a job where you sit for extended periods of time, it is important for you to get up and stretch your legs at least once every hour. While seated, you can flex your ankles to help the blood flow in your legs.
- Lifestyle changes can help prevent a blood clot from forming. You should make sure you are at a healthy weight for your age and height. Make sure to also speak with your doctor if you have a family history of pulmonary embolism. Make sure to monitor other health problems, like heart disease or lung problems that could lead to PE.
Risk of Pulmonary Embolism: Treatment Options for PE
There are a few treatments that are implemented when dealing with PE. Blood thinners and clot dissolvers may help when treating PE. Clot dissolvers are applied directly to the vein so it can break it down immediately.
If the clot is too big or life-threatening, then it is surgically removed. A vein filter may be inserted and positioned in your body’s main vein to stop clots from being carried from your legs to your lungs. This procedure is used when blood thinners and can’t be taken, or they don’t work fast enough. The filter can be removed later if it’s not needed.